The way we access healthcare is changing rapidly, and telemedicine has emerged as one of the most transformative innovations in modern medicine. No longer confined to the traditional doctor’s office, telemedicine allows patients to consult with healthcare professionals from the comfort of their homes, workplaces, or even while traveling. This shift has significant implications for convenience, accessibility, and the overall efficiency of healthcare systems worldwide.
Telemedicine isn’t just about video calls with a physician. It encompasses a wide range of services, including virtual consultations, remote monitoring, prescription management, mental health therapy, and follow-up care. By integrating technology with medical expertise, telemedicine has bridged the gap between patients and providers, enabling timely interventions, reducing hospital visits, and minimizing disruptions to daily life.
The Rise of Telemedicine
Several factors have contributed to the rapid adoption of telemedicine. Advances in high-speed internet, mobile device accessibility, and secure digital platforms have made virtual care a viable alternative to in-person visits. Additionally, the COVID-19 pandemic accelerated adoption by highlighting the risks of traditional healthcare settings and the need for remote options. Patients began seeking virtual appointments for both urgent and routine medical needs, and healthcare systems responded with scalable platforms and standardized protocols.
Telemedicine has also expanded access to healthcare in underserved regions. Rural communities, where medical specialists may be scarce or distant, can now receive timely consultations. Chronic disease management, mental health support, and preventive care have become more attainable for populations who previously faced geographic or logistical barriers.
How Telemedicine Works
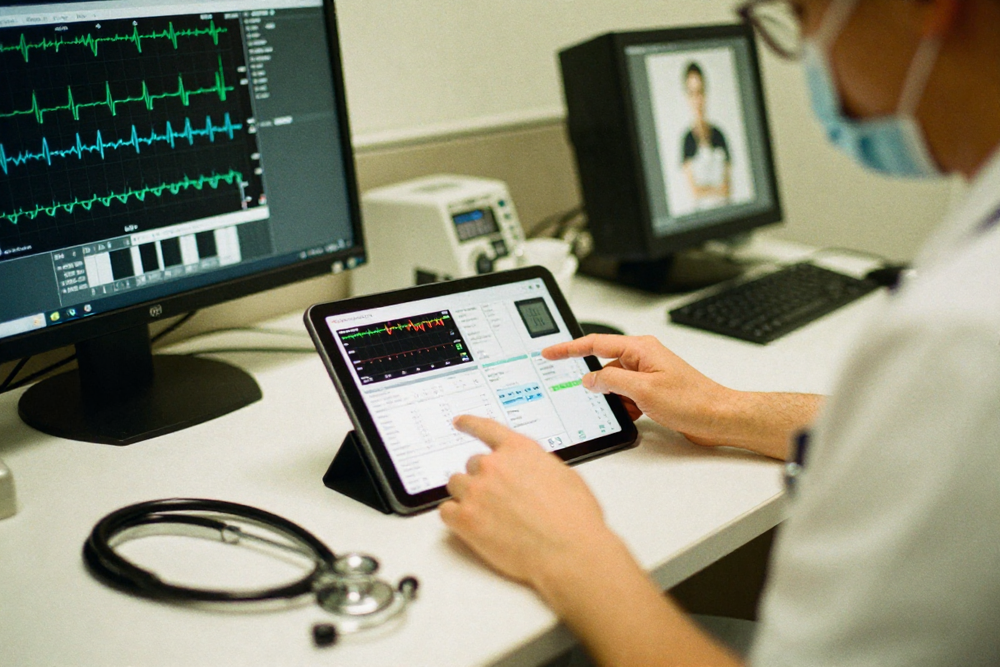
Telemedicine typically begins with a patient logging into a secure platform using a smartphone, tablet, or computer. After scheduling an appointment, they connect with a healthcare provider through video conferencing or messaging tools. The consultation can cover diagnosis, treatment recommendations, lab result review, and follow-up advice. Many platforms also provide features like electronic prescriptions, digital health records, and integration with wearable devices that monitor vital signs in real-time.
Remote monitoring has become particularly important for managing chronic conditions such as diabetes, hypertension, and heart disease. Patients can share daily readings from smart glucose meters, blood pressure monitors, or wearable trackers, allowing physicians to adjust treatment plans promptly without requiring frequent in-person visits. This continuous flow of information improves health outcomes and reduces the risk of complications.
Benefits of Telemedicine
One of the most obvious advantages of telemedicine is convenience. Patients no longer need to commute to clinics, sit in waiting rooms, or take time off work for short appointments. This convenience extends to caregivers as well, who can support family members in need without logistical challenges.
Telemedicine also promotes faster access to care. Minor health issues that might have been delayed due to scheduling or travel constraints can now be addressed within hours. Early intervention can prevent conditions from worsening, ultimately reducing the need for emergency visits or hospitalizations.
Cost savings are another significant benefit. Virtual appointments are often less expensive than in-person visits, and by reducing unnecessary travel and time away from work, patients save both money and energy. For healthcare providers, telemedicine can improve efficiency, reduce patient congestion, and allow for better resource allocation.
Moreover, telemedicine offers improved continuity of care. By centralizing medical records and making information easily accessible, patients and doctors can maintain an ongoing dialogue, monitor progress, and adjust treatments seamlessly. This continuity is particularly valuable for patients managing multiple conditions or long-term treatments.
Telemedicine and Mental Health
Mental health care has been one of the most significant beneficiaries of telemedicine. Virtual therapy sessions, counseling, and psychiatric consultations provide privacy, reduce stigma, and make accessing mental health professionals easier than ever. Patients who might struggle to attend in-person sessions due to mobility, location, or social anxiety can now receive support from their own homes.
Platforms also offer a range of services beyond video sessions, including guided meditation, stress tracking, and interactive cognitive-behavioral therapy (CBT) programs. By leveraging technology, mental health care becomes more flexible, personalized, and scalable, reaching populations that previously faced barriers to access.
Challenges and Considerations
While telemedicine offers numerous advantages, it is not without challenges. One limitation is the inability to perform certain physical examinations or procedures remotely. Diagnoses that require tactile assessment, imaging, or lab tests still necessitate in-person visits. However, hybrid models that combine virtual and physical appointments are increasingly common, ensuring that patients receive comprehensive care.
Privacy and data security are critical concerns. Telemedicine platforms must comply with strict regulations to protect patient information. Encryption, secure login systems, and robust data management protocols are essential to maintaining trust and confidentiality. Patients should choose reputable providers and platforms with strong privacy measures.
Another consideration is digital literacy and access. While telemedicine expands access for many, individuals without reliable internet, devices, or technical know-how may find it challenging to participate. Addressing these disparities is essential to ensure equitable access for all populations.
The Future of Telemedicine
Telemedicine is poised to continue transforming healthcare delivery. Integration with artificial intelligence, predictive analytics, and advanced wearable devices will enhance diagnostics, treatment personalization, and preventive care. Smart algorithms may flag health trends before they become critical, guiding patients to early interventions.
Healthcare systems are increasingly embracing telemedicine as a permanent part of their offerings, recognizing its potential to improve efficiency, patient satisfaction, and outcomes. As platforms evolve, the technology will become more intuitive, immersive, and capable of providing high-quality care across a broader range of medical specialties.
Its benefits are clear: convenience, speed, cost savings, improved continuity of care, and expanded access to underserved populations.
While challenges remain, particularly in areas requiring physical examinations and ensuring equitable access, telemedicine is a transformative tool that continues to reshape the healthcare landscape. For patients and providers alike, embracing this technology means more timely care, greater flexibility, and the ability to manage health proactively. As telemedicine grows and integrates with emerging technologies, it promises to make healthcare not only more accessible but also smarter, more responsive, and tailored to the needs of every individual.




